LARYVOX® PAD
Tracheostomy placement, i.e., the displacement or shortening of the airway, is now regularly performed in many medical specialties based on a variety of indications. Accordingly, the need for the measure may only be short-term or it may also be permanent.
Subsequent care of the tracheostoma, the opening for breathing, quite often poses special challenges for physicians, nurses, patients and relatives.
"Every person is an individual - and so is every tracheostoma."
Professional tracheostoma care is always performed with a view to the best possible adaptation of the aids to the patient's individual circumstances and needs. For example, good adaptation of the tracheostomy tube to the anatomy is important for comfortable use of the aid, as is care and maintenance of the health of the parastomal skin as well as good sealing of the tracheostoma to prevent unwanted loss of breath for a satisfactory voice result.
What are the particular challenges of providing care?
Different aspects influence the shape, size, uniformity and depth of the skin level of a tracheostoma. Even the intraoperative creation of the tracheostoma can be performed using different techniques, which then influence the later appearance of the airway opening. Subsequent radiation therapy may also impact skin structure or tracheostoma size over time. These can be both permanent or of a temporary nature. Even the use of the tracheostomy tube and its fixation with a tube holding strap can, under certain circumstances, lead to a change in the shape of the tissue if handled incorrectly.
Typical problems occur at different times in patients and not infrequently require a very individualised supply of aids, which sometimes only produces the desired results after multiple product changes. For example, a deeply positioned, irregular tracheostoma is difficult to care for as no sealing effect can be achieved with the tracheostomy tube, or the base plates cannot find an even contact surface to provide the longest possible hold.
"Lösungsalternativen kann LARYVOX® Pad in verschiedenen Ausführungen bieten."
The self-adhesive, skin-coloured silicone pads are used to adjust the skin level of an irregular tracheostoma. Their high degree of suppleness ensures good placement on the tracheostoma and may possibly provide an optimised support surface for a base plate.

LARYVOX® PAD

LARYVOX® PAD CONNECT
Application
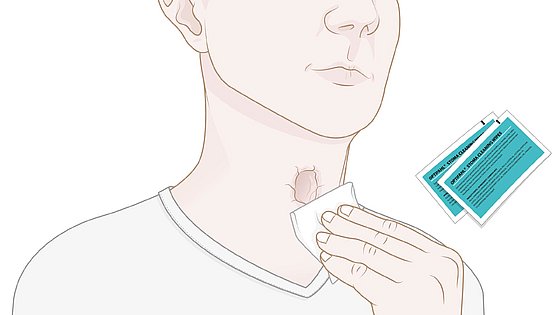
1. Clean, degrease and dry the parastomal skin (the skin surrounding the tracheostoma) with an OPTIFAHL® stoma cleaning wipe.
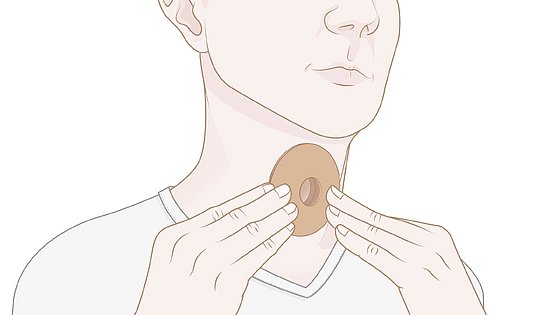
3. Fix the LARYVOX® PAD with slight pressure around the stoma.
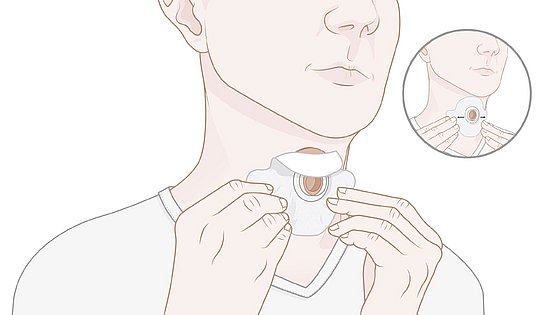
5. With a LARYVOX® PAD/LARYVOX® PAD PRO, a base plate must also be glued to the PAD to use an HME.
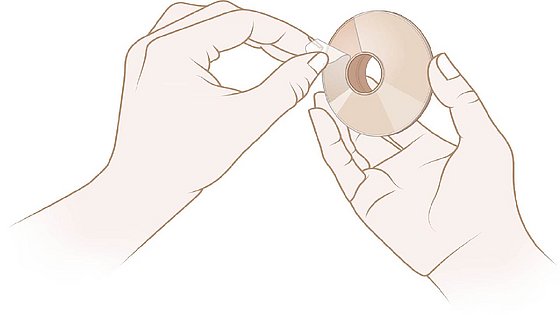
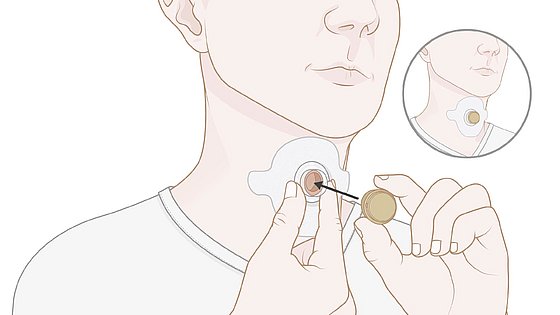
2. Remove the protective film from the back of the LARYVOX® PAD.
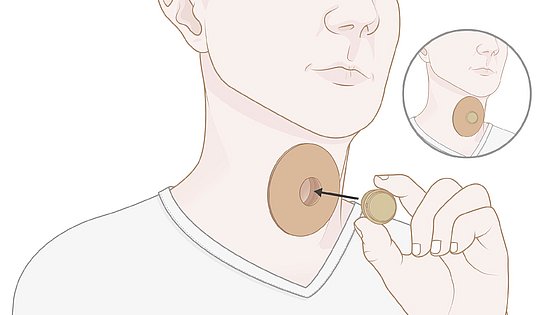
4. With a LARYVOX® PAD Connect, an HME can be attached directly via the integrated 22 mm combi-adapter.